Introduction For years, risk adjustment followed a predictable playbook: meet deadlines, prepare for annual RADV, and repeat. The new MA RADV audit cycles have rewritten that playbook entirely. In 2026, health plans are simultaneously managing five overlapping MA RADV audit cycles — Payment Years 2020 through 2024
Read More →Why element-level scoring is the new hurdle for SNPs As we navigate the long and winding road of 2026, a new deadline is fast approaching: the May 2026 submission window for CY 2027 guidelines. The Model of Care (MOC) has evolved into a high-stakes precision test where
Read More →The landscape of Medicare Advantage (MA) Risk Adjustment Data Validation (RADV) has undergone a seismic shift. CMS is no longer just sampling the industry; they are auditing every eligible contract, every year. With federal estimates indicating roughly $17 billion in annual overpayments due to unsupported diagnoses, the
Read More →By Regan Pennypacker, MSL, CCEP As we turn the calendar to February, the fast-moving pace of the new year shows no sign of a slowdown. The classic tune “Under Pressure” resonates more than ever within our industry. Organizations across the country are holding their breath while waiting
Read More →CMS recently released updated operational guidance for Contract Year (CY) 2027 Medicare Advantage (MA) applications. This guidance introduces pivotal shifts in how organizations manage network adequacy and exception requests, meaning the “old way” of managing deficiencies is no longer sufficient for those preparing for the February submission.
Read More →We are pleased to announce the appointment of Regan Pennypacker, MSL, CCEP, to our executive leadership team as Senior Vice President, Compliance Solutions. Regan is a recognized leader in managed care and regulatory affairs with over 25 years of experience driving strategic compliance initiatives and operational excellence
Read More →In the Contract Year 2027 Proposed Rule (CMS-4212-P), CMS introduced significant changes to how provider network changes are handled, which will directly impact health plan operations and enrollment stability. For health plan leaders, the headline is clear: the proposed changes remove historical guardrails around network stability, potentially
Read More →As we close out 2025, the first year of mandatory secret shopper surveys under the CMS Final Rule is behind us. With the 2026 cycle starting on January 1, now is the time to apply the hard-won lessons from the inaugural reporting year. Reviewing the 2025 Access
Read More →Major regulatory forces, from RADV extrapolation to new payment models, are converging. Here is why the next 18 months represent the most significant operational transformation in a decade. The Medicare Advantage sector is facing its most significant operational transformation in a decade. We are no longer looking
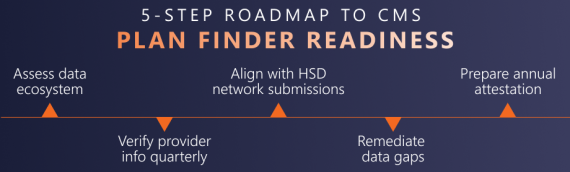
Read More →CMS Finalizes Medicare Plan Finder 2027 Rule: What Health Plans Need to Know In one of the most consequential transparency updates in recent years, CMS has finalized new requirements that will make Medicare Advantage (MA) provider directories publicly available on Medicare Plan Finder beginning with plan year 2027. This change marks a
Read More →